Which Is an Obstacle to Peer Review Activities?ã¢â‚¬â€¹
The collection of ethnicity data has been demonstrated to be important in healthcare. Even so, despite recent efforts by the U.k. regime, it remains incomplete and unvalidated. In order to exist able to assess inequalities and target resources appropriately, it is essential to have complete and accurate data. This paper examines the reasons for the gaps in ethnicity data based on the perceptions and experiences of the healthcare professionals who are charged with collecting these data. A questionnaire was used to assess perceptions of ethnicity data collection, including whatever barriers encountered as well as the perceived importance of collecting these data.Respondents were askedwhether routine ethnicity data collectionwas limited to specific affliction areas, and pproximatelywhat proportion was complete in these areas. There were also questions concerning preferred methods of collection (east.g. cocky-report). The questionnairewas completed by 30 respondents, who included healthcare managers, clinicians, nurses and other staff working in the healthcare setting. The findings confirmed that the collection of patients' ethnicity data is deemed of import by the healthcare professionals, but showed that there remains incertitude and unease as to how best to collect these data or how to explain to patients how the information will exist used. The majority of healthcare professionals agreed that it was of import to record patients' ethnicity, but no clear rationale was given to staff about the use of these information, and no grooming was provided on the best manner to collect the data.
What is known on this subject
• Inequalities in wellness and admission to healthcare among ethnic minority groups have been widely reported. Nevertheless, ethnicity data drove to engagement has frequently been conducted in an ad-hoc manner, resulting in patchy information.
• The need for good-quality and consummate ethnicity data has been reinforced by the Equality Act 2010, which places responsibility on government to tackle inequalities and target services accordingly.
• Many authors emphasise the need for improved ethnicity data collection and monitoring, but little is known nearly the barriers that healthcare professionals face up when collecting these information.
What this paper adds
• It provides a rare glimpse of the barriers to ethnicity data collection equally revealed by healthcare professionals who are not collecting the data, and a meliorate understanding of the problems experienced by those who practise collect them.
• The barriers identified here point to areas in which the development of preparation materials is vital.
Key words
data collection, ethnicity, healthcare professionals, perspectives
Introduction
The 2001 UK demography classified four.6 million people equally belonging to a non-white ethnic grouping (7.9%) ,with over 50% of these being Asian or British Asian (Office for National Statistics, 2001). Reports on health inequalities and outcomes past ethnic group emphasise the necessity of overcoming barriers to brand fashion for complete and accurate recording of ethnicity. Some indigenous groups have an increased incidence of specific diseases, such equally some cancers, and experience disparities in access to both primary and secondary services (Chinegwundoh et al, 2006; Bowen et al, 2008; Sproston and Mindell, 2006; Jack et al, 2009, 2010, 2011; Farooq and Coleman, 2005; Atkinson et al, 2001; Aspinall and Jacobson, 2004). Furthermore, certain ethnic minority groups are associated with risky behaviours. For instance, smoking rates are reported to be highest in Bangladeshi males, at 44%, compared with 27% in the general population (White, 2002).
Policies based on inaccurate data may lead to poor targeting of resources and services (White, 2002; London Health Observatory, 2003; Mackintosh, 2005). In this testify-based era, the reality neatly stated by Johnson is 'that which is measured tin be aimed at; that which is left unobserved can be ignored' (Johnson, 2012, pp. 39–twoscore).
UK government policy beginning required ethnicity data collection for Hospital Episode Statistics (HES) in 1995. However, loftier levels of missing data and invalid codes in the early years made the data unusable (Aspinall, 2000). Although there has been some comeback, such as the decline of 'not known' or 'non stated' codes in Finished Consultant Episodes from 23.ix% in 2004–2005 to 8.half dozen% in 2009–2010, HES data remain incomplete (HESonline, 2009). In 2004, the Quality and Outcomes Framework (QoF) began awarding one bespeak (of a possible 1000 points) to GP practices for the recording of ethnicity for all newly registered patients. The incentive was insubstantial, and uptake was limited and was therefore later on abandoned (Johnson, 2012).
In 2005, the Section of Health produced A Practical Guide to Ethnic Monitoring in the NHS and Social Care (Department of Health, 2005b). An ethnic monitoring tool developed by NHS Scotland was also released in 2005. The tool offered information on the 'whys' (duty and accountability) and 'hows' of indigenous monitoring (i.e. who is involved and what needs to be put in place). Grooming materials were available to download and modify aslope 'Training the Trainer' notes and function-play scenarios (NHS Wellness Scotland, 2005). However, footling is known about the practical applicability and uptake of any of these guidelines.
The Equality Act 2010 reinforced the Race Relations Human action of 1976 and the subsequent Subpoena in 2000. This legislation made public authorities direct responsible for ensuring disinterestedness in access to healthcare and for reducing inequalities. Furthermore, public authorities are required to publish information to demonstrate their adherence to the legislation and to set articulate objectives for the time to come. The intention is that compliance with the legislation will lead to a improve understanding of the controlling processes and make public government answerable for their performance (Home Office, 2010).
Staff attitudes to ethnicity data collection have been reported to be quite positive (Pringle and Rothera, 1996). For example, a survey of xvi GPs and practice managers reported that they all regarded ethnicity information collection favourably and thought it adequate, practical and beneficial for service evaluation and targeted health promotion equally well as for other purposes (Sangowawa and Bhopal, 2000). Nevertheless, ethnicity data drove is known to be patchy, particularly in primary care, where much of the inquiry has focused upon the acceptability, feasibility, resource implications (including staff time), and limitations of estimator systems, categories and coding (Kumarapeli et al, 2006; Pringle and Rothera, 1996).
In our starting time publication about this research nosotros reported findings from a systematic literature review of ethnicity data collection methodology in primary and secondary intendance (Iqbal et al, 2009). 'Barriers to collection' featured every bit one of seven themes that were identified, and the evidence revealed healthcare professionals' perceptions to be a major obstacle to the collection of ethnicity data. Fearfulness of causing offence to patients or encountering resistance, together with confusion about ethnicity categories and a lack of understanding of the need for ethnicity data, have also been reported as deterrents by healthcare professionals in two reports from the USA (Hasnain-Wynia et al. 2004; Regenstein and Sickler, 2006). Baker et al (2005) reported that administrative staff feared that asking for ethnicity information would alienate patients. Barriers reported past US physicians included the beliefs that collecting ethnicity data would be time consuming, would impinge on privacy and would be uncomfortable for both staff and patients, only the greatest barrier was the belief that the data had no relevance (Wynia et al, 2010).
In our second publication nosotros reported the results of a series of focus groups conducted with healthy S Asian volunteers (Iqbal et al, 2012). The topic guide focused on perspectives and experiences of ethnicity information collection in a healthcare setting. The findings showed a somewhat linear relationship between staff comfort and patient willingness, such that the more than comfortable the staff appeared to exist about asking the question, the morewilling the patients were to provide these data. The participants also felt that staff should be able to offering reasons for collecting the information and explanations of how the data would exist used. In a U.s.a. written report, Baker et al trialled four unlike rationales and institute that patient comfort levels were highest when quality monitoring was cited as the reason for collection (Baker et al. 2005).
Despite the push towards improving the abyss and reliability of ethnicity data recording, little is known about how healthcare professionals in the United kingdom perceive the collection of these data. The aim of this paper is to explore the likely reasons for gaps in the ethnicity information by evaluating the perceptions and experiences of healthcare professionals who are tasked with collecting this data.
Methods
Cancer Research UK commissioned a project to assess ethnicity data collection for statistics relating to cancer incidence, direction, mortality and survival in the U.k.. Upstanding blessing was obtained from South Birmingham Inquiry Ethics Committee.
A survey of healthcare professionals was undertaken using a questionnaire based upon 1 previously developed by the Middle for Prove in Ethnicity, Health and Multifariousness (CEEHD), and modified past the project working group. The modified questionnaire consisted of nine items using a mixed style of questions. Respondentswere asked to rate how important they idea the drove of ethnicity data was using Likert-style items, while other questions were posed in either a airtight format (no/yes/not known response options) or a tick-box format. Two open-ended questions were included, assuasive respondents to provide detailed reasons for not recording ethnicity and to describe whatsoever issues encountered. The questionnaire was intended for clinicians, managers, nurses and other staff (eastward.g. reception staff) involved in collecting or using ethnicity data in a healthcare setting (see Figure i).
The questionnaire was distributed between March and June 2007 throughout England and Wales, via the Minority-Ethnic-Health and ALLSTAT JISCMail lists (a national academic mailing list service for academic and research communities). Questionnaires were as well circulated to the 23 Race for Health primary intendance trust programme leads, equally well as to all registered members of the Race for Health mailing list. The questionnaire was posted on the CEEHD website with a link to this placed on the NHS Evidence – Ethnicity and Healthwebsite (formerly the Specialist Library forEthnicity and Wellness) and sent to the National Cancer Enquiry Network (NCRN) head part for apportionment to the 24 Cancer Networks in England and Wales. A thread was created on NHS and Academic Clinical Oncology and Radiobiology Inquiry Network (ACORRN) word forums. Regular weekly bulletins from the NHS forum to its members highlighted new threads. The questionnaire could be completed and returned past either post or email. In total, 14 questionnaires were completed and returned within the 4-week borderline. Thiswas extended for a further 4 weeks (on the website links). Circulation of the questionnaire to the NCRN was repeated, but this time the questionnaire was sent electronically to each network director, which increased the number of questionnaires returned to 30. There was a special interest in the cancer networks because the project was commissioned past Cancer Research Great britain.
Results
In full, 30 responses were received, coded, analysed and reported using descriptive statistics. Responses to the open questions reasons why ethnicity information are non collected and issues encountered when collecting these data are presented every bit direct quotations. Respondents classified themselves every bit clinicians (north = vii), nurses (n = 5), managers (n = 5), information scientists (n= six) and other (due north = 7), which included ii radiographers, a cancer services coordinator, a patient profiling officer, a quality coordinator, a diabetes educator and a diversity managing director.

Effigy 1: Ethnicity, Health and Diverseness questionnaire
In total, 21 respondents (70%) attempted to routinely collect some form of ethnicity data, two (seven%) did not consistently collect ethnicity data, and seven (23%) did not collect any ethnicity data. Respondents who collected ethnicity data (routinely or occasionally) did so for cancer (37%), for all illness areas (32%) or for diabetes and hypertension (5%). The majority used the recommended self-study method (north = 12); observer cess was used less often (n = 4). Several respondents reported using a combination of methods (e.g. self-written report and observer assessment) (see Figure two).
Respondents who did not collect ethnicity data were asked to give their reasons for this. Their explanations included a lack of resource:
Our data drove is poorly resourced as it is, so we have to stay entirely focused on what is clinically relevant. (Oncologist)
It is very hard to tape ethnicity data for our cancer records as it is not documented in the patient's case notes, to the best of my noesis. Due to this, it would take a great bargain of fourth dimension to collect and is, yet, not asked for in any reports that are asked of me. (Cancer professional person)
Respondents stated that they were not required to collect or study ethnicity data:
Ethnicity data is non part of the data sets that are collected. (Information director)
In some instances, ethnicity data were only collected for specific services or when requested every bit part of a clinical trial:
Ethnicity data drove currently limited to midwifery as Trust is taking part in the Welsh Assembly Authorities Patient Equality Monitoring Project and staff are pending training in how to collect information. (Homo resources manager)
Only if it is required as part of a research trial and the company require that information. We then but fill it in, just information technology is very rare. We do not routinely collect this. (Research nurse)
Collecting ethnicity data could be problematic:
because information technology involves request the patient what they want it to exist and they are not always available or willing to answer. (Information science pb)
Staff collecting ethnicity data might not be enlightened of the need for self-report, and patients might refuse to answer if the options available did not match their ethnicity. Ethnicity was most commonly recorded based on the categories used in the Census (Function for National Statistics, 2001). Information about religion and language were routinely nerveless, simply data almost country of origin, race and country of nascency were to the lowest degree likely to exist collected (see Effigy three). Information systems were reported to be inadequate, and the ethnicity categories needed to be refreshed:
Existing data drove systems are non made for it. Ethnic categories are non upwards to date, follow erstwhile traditional immigration routes. (Data analyst)
Collected as part of a large data fix, and some items are poorly returned. (Chair of data network)
The optional nature of ethnicity information drove was an additional cistron. Patients could choose not to answer, which meant that ethnicity data would e'er be incomplete.
Ethnicity data collection was considered:
Fourth dimension consuming – reception time, patient fourth dimension, information entry time, also language have used link workers to assist patients fill up in. Definite resource implications. (GP)
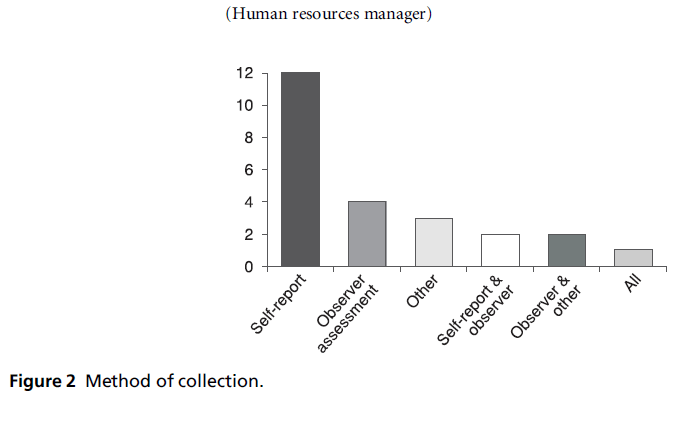
Figure 2: Method of drove.

Figure three: Routinely collected indicators.
Patients and staff did non always empathize why it was necessary:
Nosotros have been collecting data surrounding ethnicity, etc. for around 7 years. The main issue is the patients' lack of understanding of what ethnicity is. Besides practise staff 's lack of awareness of why we need to collect this information. On the whole, though, there have been very few problems. (Patient profiling development officeholder)
Ease of admission to information was as well a problem. Ethnicity information were not always recorded in an accessible place, such as the front of the patient's records or on the reckoner, which could mean that it was necessary to manually search for the information:
Often not recorded on software, so had to retrieve sometime notes and read through pages of clerking notes. Ethnicity usually recorded by junior doctors + written in. I did not wish to presume ethnicity from name lone. (Consultant)
Staff feared being challenged by patients who wanted to know the reasons for the collecting of ethnicity data, and the possibility of ensuing hostility, or causing offence:
Patients will ask why y'all need to know. If they come for anonymous info [they] do not want to be listed. Do not accept that you need to have an idea of ethnic origin and so every bit to be able to review/develop/alter service that is provided. (Information and back up services manager)
I experience this is a difficult area due to fear of offending anyone. Most of the younger generation are British, I would have thought. (Nurse)
Training large workforces was problematic:
We have had difficulty releasing the vast numbers of staff required to attend 'patient equality monitoring' training sessions. However, this has been made easier by an All- Wales Patient Equality Monitoring Projection sponsored by the Welsh Associates Government and run past the NHS Wales Heart for Equality and Human Rights, who have produced an excellent Train the Trainer pack for patient equality monitoring. (Manager)
Still, the situation had changed following the development of a Train the Trainer pack by the NHS Wales Middle for Equality and Man Rights. Finally, respondents were asked to charge per unit how important they personally thought ethnicity data collection was, and how important they perceived information technology to be to their organisation. Overall, respondents attached more importance to it at a personal level (69%) than at an organisational level (59%). This may exist due to a lack of training provision. Only 28.5% reported that their organisation provided ethnic monitoring training, 28.v% reported that no training was provided, and the remaining 43% were not enlightened of whatsoever training provision. In total, 12 respondents (44%) expressed an involvement in attending a workshop on ethnic data monitoring and its uses in cancer.
Give-and-take
These findings showed that, although individuals regarded ethnicity information drove as of import, this did not mean that they went on to really collect this data. A number of barriers were identified, particularly that of using cocky-report, which is unanimously agreed to be the ideal method of drove and is recommended by many guidelines equally the golden standard (Commission for Racial Equality, 2002; Department of Wellness, 2005b; Regenstein and Sickler, 2006). However, assessment by observation alone based upon advent (e.g. skin color, hair color and/or type, apparel code), despite existence discouraged, was the second most commonly utilised method. Reasons given for using this arroyo included the abstention of discomfort and confrontation, accompanied by a fear of causing offence to patients. This is not a new concern. An early experimental projection on collecting ethnicity data in the NHS recorded a similar fear of offending patients coupled with a fear of being accused of bigotry, embarrassment when asking the questions, and concern that the questions were besides sensitive as the master barriers to ethnicity data collection (Johnson et al, 1993). In the modern context, worries emerged virtually dealing with younger patients who are more than likely to be built-in in theUKand who may wish to identify themselves as British. In add-on, one respondent in our survey highlighted the difficulty of obtaining self-reported ethnicity data (as recommended by Department of Health guidelines) in situations where the patient is unwilling or just chooses non to provide the information (Department of Health, 2005a).
Methods of information collection other than self-report are actively discouraged by the Commission for Racial Equality, and may merely be used where cocky-written report is non possible. Results of surveys conducted by the Robert Wood Johnson Foundation (a funding torso established in the United states of america in 1972) revealed that 61% of healthcare professionals used the self-written report method, whereas 25% used the observer method. Professionals considered the information to exist accurate, given their cognition of the local population, and believed that this method eliminated discomfort both for themselves and for the patients (Regenstein and Sickler, 2006).
A number of our respondents did non endeavor to collect whatever form of ethnicity information. In many cases this stemmed from their own or their system'due south lack of awareness of the importance of the information, and the belief that it was non relevant to patient care or treatment. Even so, exceptions occurred if the information was required for participants in a clinical trial or for religious, dietary or communication purposes. Interviews conducted with physicians in the Us revealed that the strongest objection to collecting ethnicity and race data is the belief that information technology is, or should exist, clinically irrelevant. Other barriers that were reported included a lack of resource, concerns about privacy, the legality of collection, and discomfort or resistance on the part of patients and staff (Hasnain- Wynia et al, 2010). These findings concur with the earlier results reported by Regenstein and Sickler (2006), who establish that the single most important barrier to information drove is staff not knowing why information technology is important. However, this was not reflected in our sample, where only one participant expressed the view that information technology was 'not relevant to intendance or treatment.'
Additional barriers that were reported included difficulty in allowing staff time away from work to attend off-site training courses. However, training packages such as those developed by Lambeth Primary Care Trust, NHS Wellness Scotland, and the Wellness Inquiry and Educational Trust (HRET) in the USA freely offering a wide range of fabric online, including role-play scenarios which tin be used for in-firm training (NHS Health Scotland, 2005; Health Research and Educational Trust, 2007; Race for Health, 2006). Weinick et al. (2007) take found 'railroad train the trainer' sessions to be a feasible alternative to releasing numerous staff for training in Massachusetts in the U.s..
Instance of adept practice
Lambeth Master Intendance Trust is an example of practiced practice where ethnicity monitoring has been relentlessly pursued. Lambeth introduced the 'Individual Patient Registration Contour' program, which provided substantial greenbacks injections to GP practices as an incentive to collect comprehensive patient profiling data, and also provided i.five days of staff training, with the one-half 24-hour interval being held at the practice. Practices were also assisted with patient profiling data collection for all patients. Mailshots of the profiling questionnaire were posted out to capture data for registered patients with free return envelopes and fully funded data entry upon return. Data were nerveless prospectively for all new registrations and recorded on dedicated templates provided past the programme. The resulting data have been used in a wellness equity audit of End Smoking Services and a needs assessment exercise undertaken with the Portuguese customs (Race for Health, 2006).
Regenstein and Sickler (2006) accept provided examples of skillful practice in the Us, which include the provision of ethnicity information collection training for new hospital employees as role of their consecration programme. Furthermore, members of staff working in registration areas are subjected to a quality review. Managers are able to identify individuals who record a large number of 'unknown' ethnic categories or fail to record whatever ethnicity data, and and so provide farther grooming where necessary.
Limitations
This study was limited in terms of fourth dimension and resources, and we were therefore unable to recruit a big sample or comport large mailshots, but relied instead on links to the questionnaire posted on websites, forums, newsletters and mailing lists, and a pocket-sized mailshot to allNCRN network managers.Unfortunately, thismeans that we are unable to calculate a response charge per unit. In the event, we received only 30 responses despite extending
the borderline for returns. With hindsight, an online questionnaire would take been easier to complete. Information technology would have eliminated the need to print out, post or email the completed questionnaire, and might have resulted in an increased response rate. Targeted mailshots such as that to theNCRNcould accept been sent to other groups (e.one thousand. individual GP practices or principal care networks), which might have yielded more questionnaire returns than using JISCMail lists. However, given the scarcity of research in this area, the responses that nosotros did receive provide a useful insight into the perceptions and experiences of healthcare professionals today, and identify important areas for farther consideration.
Conclusion
Our findings are likely to be irrelevant without a change in local and national policy. Ethnicity information drove needs to be mandated in master intendance and improved in terms of quality and completeness in secondary care. Grooming exercises should include familiarising healthcare professionals with the Equality Act 2010, and raising sensation of the need for ethnicity data drove and how these information volition be used. Methods of drove should also exist included, and the importance of self-study emphasised, too as the demand for standardising of the rationale, wording of questions, response categories offered, and answers and explanations to ofttimes asked questions. Training may help to alleviate any anxiety felt past staff who are tasked with obtaining ethnicity data frompatients. It should be emphasised that using the data we already have, irrespective of its quality and abyss, will encourage improved drove by highlighting any inadequacies. Unused data are a disincentive to healthcare professionals and patients alike (Iqbal et al, 2012; Fulton, 2010).
In conclusion, 'wellness equality is non possible without ethnic monitoring' (Fulton, 2010, p. 5). Improving ethnicity information collection requires commitment from governing bodies and agreement on what is to be collected and when. Standardised questions should be complemented by sufficiently flexible options to facilitate responses from those who exercise non quite fit predetermined categories. Patients need to feel assured that these data will exist treated confidentially and used appropriately (Johnson, 2012; Fulton, 2010). Ethnicity information are of no value if they are not utilised to target resource and reduce inequalities (Raleigh, 2008).
A few primary intendance trusts have worked hard to meliorate ethnicity data collection, and have utilised the resulting data to help to reduce wellness inequalities (Race for Health, 2006; Public Health Sector, School of Health and Human Sciences, Liverpool John Moores University, 2000). However, these are isolated examples. What is needed, aslope these efforts, is a consequent message from policy makers and managers to frontline staff that collecting these data matters. Ethnicity data collection should be function of the daily routine at both main and secondary care levels. Almost importantly, nosotros need more reporting of ethnicity data in healthcare in order to better planning and delivery of services for members of ethnic minority groups.
Acquittance
The authorswould like to thank all of the respondents, without whom this research would not have been possible. We would also similar to thank the Informational Board for their input into this project. This work was commissioned and funded by Cancer Research UK, and we would similar to thank Vanessa Gordon-Dseagu, Catherine Foot and Ruth Yates for their support throughout the projection.
References
- Aspinall P (2000) The mandatory collection of data on ethnic group of inpatients: experience of NHS trusts in England in the get-go reporting years. Public Health 114:254ÃÆ'ƒÂ¢ÃÆ'‚€ÃÆ'‚“nine.
- Aspinall PJ and Jacobson B (2004) Ethnic Disparities in Health and Health Care: a focused review of the evidence and selected examples of practiced practice. London: London Health Observatory.
- Atkinson M, Clark M, Clay D et al (2001) Systematic Review of Ethnicity and Health Service Access for London. London: Regional Office, NHS Executive.
- Baker DW, Cameron KA, Feinglass J et al (2005) PatientsÃÆ'ƒÂ¢ÃÆ'‚€ÃÆ'‚â„¢ attitudes toward health care providers collecting data about their race and ethnicity. Journal of General Internal Medicine 20:895ÃÆ'ƒÂ¢ÃÆ'‚€ÃÆ'‚“900.
- Bowen R, Duffy S, Ryan D et al (2008) Early onset of breast cancer in a group of British blackness women. British Periodical of Cancer 98:277ÃÆ'ƒÂ¢ÃÆ'‚€ÃÆ'‚“81.
- Chinegwundoh F, Enver Grand, Lee A et al (2006) Risk and presenting features of prostate cancer amongst African- Caribbean area, S Asian and European men in North-east London. BJU International 98:1216ÃÆ'ƒÂ¢ÃÆ'‚€ÃÆ'‚“20.
- Commission for Racial Equality (2002) Ethnic Monitoring: a guide for public government. London: Commission for Racial Equality.
- Department of Wellness (2005a) Department of Health Race Equality Scheme: 20052008. London: Section of Wellness.
- Department of Wellness (2005b) Practical guide to Indigenous Monitoring in the NHS and Social Care. London:
- Department of Wellness.Farooq S and Coleman MP (2005) Breast cancer survival in S Asian women in England and Wales. Journal of Epidemiology and Community Health 59:402ÃÆ'ƒÂ¢ÃÆ'‚€ÃÆ'‚“half dozen. 290
- Grand Iqbal, MRD Johnson, ASzczepura et al Fulton R (2010) Ethnic Monitoring: is health equality possible without it? Better Wellness Briefing Paper 21. London: Race Equality Foundation.
- Hasnain-Wynia R, Pierce D and Pittman M (2004) Who, When, and How: the current state of race, ethnicity, and primary language data collection in hospitals. New York: The Democracy Fund.
- Hasnain-Wynia R, Van Dyke K, Youdelman M et al (2010) Barriers to collecting patient race, ethnicity, and main language data in doc practices: an exploratory report. Journal of the National Medical Association 102: 769ÃÆ'ƒÂ¢ÃÆ'‚€ÃÆ'‚“75.
- Health Enquiry and Educational Trust (2007) HRET Disparities Toolkit: a toolkit for collecting race, ethnicity, and primary linguistic communication information for patients. www.hret disparities.org
- HESonline (2009) How Good is HES Ethnic Coding and Where Practise The Issues Lie? Leeds: Health and Social Intendance Information Centre. www.hesonline.nhs.uk/Ease/ servlet/ContentServer?siteID=1937&categoryID=171
- Home Office (2010) Equality Act 2010. London: Dwelling Role.
- Iqbal Yard, Gumber A, Johnson Chiliad et al (2009) Improving ethnicity data collection for wellness statistics in the Uk. Diversity in Wellness and Care 6:267ÃÆ'ƒÂ¢ÃÆ'‚€ÃÆ'‚“85.
- Iqbal M, Johnson MRD, Szczepura A et al (2012) UK ethnicity data collection for healthcare statistics: the South Asian perspective. BMC Public Health 12:243.
- Jack RH, Davies EA and Moller H (2009) Chest cancer incidence, stage, treatment and survival in ethnic groups in South East England. British Journal of Cancer 100: 545ÃÆ'ƒÂ¢ÃÆ'‚€ÃÆ'‚“50.
- Jack RH, Davies EA and Moller H (2010) Prostate cancer incidence, stage at diagnosis, handling and survival in ethnic groups in S-Due east England. BJU International 105:1226ÃÆ'ƒÂ¢ÃÆ'‚€ÃÆ'‚“30.
- Jack RH, Davies EA and Moller H (2011) Lung cancer incidence and survival in different ethnic groups in South East England. British Journal of Cancer 105:1049ÃÆ'ƒÂ¢ÃÆ'‚€ÃÆ'‚“53.
- JohnsonM(2012) Issues and barriers in the collection of ethnicity and migration related data. In: Ingleby D, Krasnik A, Lorant V et al (eds) Health Inequalities and Take chances Factors Among Migrants and Ethnic Minorities. Antwerp:
- Garant.Johnson MRD, Hardman C and Jones A (1993) Developing the Implementation of Indigenous Monitoring: final report to the Home Office. Warwick: EMDP and Centre for Research in Indigenous Relations, Warwick University.
- Kumarapeli P, Stepaniuk R, De Lusignan S et al (2006) Ethnicity recording in general practice figurer systems. Journal of Public Wellness 28:283ÃÆ'ƒÂ¢ÃÆ'‚€ÃÆ'‚“7.
- Public Health Sector, Schoolhouse of Wellness and Human Sciences, Liverpool John Moores Academy (2000) Ethnicity Profiling in Primary Care: the Princes Park Wellness Centre model. Liverpool: Public Health Sector, School of Health and Human being Sciences, Liverpool John Moores University.
- London Health Observatory (2003) Variety Counts. Ethnic health intelligence in London: the story so far. London: London Health Observatory.
- MackintoshM(2005) London the globe in a urban center: an assay of 2001 Census results. London: Data Management and Analysis Grouping, Greater London Authorization.
- NHS Health Scotland (2005) Ethnic Monitoring Tool.www. isdscotland.org/isd/files/Indigenous%20MONITORING %20TOOL.pdf
- Office for National Statistics (2001) Uk Demography 2001.www. statistics.gov.uk/census2001/census2001.asp
- Pringle 1000 and Rothera I (1996) Practicality of recording patient ethnicity in general practice: descriptive intervention study and mental attitude survey. British Medical Journal 312:1080ÃÆ'ƒÂ¢ÃÆ'‚€ÃÆ'‚“82.
- Race for Health (2006) Lambeth Percent Peer Review. Liverpool: Race for Health.
- Raleigh V (2008) Collection of data on ethnic origin in England. British Medical Journal 337:a1107.
- Regenstein Thou and Sickler D (2006) Race, Ethnicity, and Language of Patients: hospital practices regarding drove of information to accost disparities in health intendance. Princeton, NJ and Washington, DC: The Robert Forest Johnson Foundation and the National Public Health and Hospital Establish.
- Sangowawa O and Bhopal R (2000) Can we implement indigenous monitoring in primary health care and use the data? A feasibility report and staff attitudes in N East England. Public Health Medicine 2:106ÃÆ'ƒÂ¢ÃÆ'‚€ÃÆ'‚“viii.
- Sproston K and Mindell J (eds) (2006) Health Survey of England 2004. Book 1.The wellness of minority indigenous groups. Leeds: Health and Social Care Data Centre.
- Weinick RM, Caglia JM, Friedman Eastward et al (2007) Measuring racial and ethnic wellness intendance disparities in Massachusetts. Health Affairs 26:1293ÃÆ'ƒÂ¢ÃÆ'‚€ÃÆ'‚“302. White A (2002) Social Focus in Brief: ethnicity. London: Office for National Statistics.
- Wynia MK, Ivey SL and Hasnain-Wynia R (2010) Drove of data on patientsÃÆ'ƒÂ¢ÃÆ'‚€ÃÆ'‚â„¢ race and indigenous grouping by dr. practices. New England Periodical of Medicine 362:846ÃÆ'ƒÂ¢ÃÆ'‚€ÃÆ'‚“50.
bermudezlicninhat.blogspot.com
Source: https://www.primescholars.com/articles/ethnicity-data-collection-in-the-uk-the-healthcare-professionals-perspective-94559.html
0 Response to "Which Is an Obstacle to Peer Review Activities?ã¢â‚¬â€¹"
Post a Comment